Antimicrobial-resistant pathogens
Towards concerted, accelerated international workflows
Investigators involved: Martina Schmidt, Xuelin Han, Li Han
Antimicrobial resistance (AMR) is an increasingly pervasive problem worldwide, and represents one of the greatest challenges to global public health today. The World Health Organization (WHO) released a new report on AMR, saying that resistance to common bacteria has reached alarming levels in many parts of the world. In some settings, few, if any, of the available treatments options remain effective for common infections. For example, the recent discovery that the mcr-1 resistance gene is spreading in China echoes news from 2010 of another so-called "superbug" gene, blandm-1, which emerged in India and rapidly spread globally.
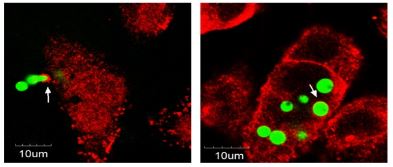
We will focus on Acinetobacter baumanni as a gram-negative coccobacillus that during the past three decades has emerged from an organism of questionable pathogenicity to a significant infectious agent in hospitals worldwide. Most alarming is the organism’s ability to adopt diverse mechanisms of resistance, the emergence of strains that are resistant to all commercially available antibiotics, and the lack of new antimicrobial agents in development. Resistance mechanisms that are expressed frequently in nosocomial strains of Acinetobacter include β-lactamases, alterations in cell-wall channels and efflux pumps. Acinetobacter is a serious pathogen in Chinese hospitals, especially with the emergence and spread of problematic strains such as NDM-1 and carbapenemase-producing isolates. Invasive pulmonary aspergillosis (IA) is the most frequent life-threatening mold infection that complicates immunosuppressive treatments (primarily hematological malignancy and intensive care unit patients) and (lung) transplantation. IA affects approximately 600 patients in the Netherlands and an estimated 36,000 in China each year. The azole drug family is the mainstay for the prevention and therapy of Aspergillus diseases, reducing mortality rates from 70% to below 30%.
To understand the mechanisms and epidemiology of AMR emergence and transmission we will - in collaboration with the Medical Microbiology - we will focus on next generation sequencing of clinically derived samples. In parallel to the NGS study, we will also create a microfluidics platform to enable the study of patient-derived material. We will create a robust model system to study the effect of small molecule inhibitors on Aspergillus infection in the lung, with a particular emphasis on allergic bronchopulmonary aspergillosis (ABPA), invasive pulmonary aspergillosis ( IPA) and angio-invasive aspergillosis (AIA). This model system will be used to test the efficacy of a number of potential treatment targets, including the cofilin:phospholipase D1 interaction. This approach will depend on cell biology, biochemistry, biophysics and molecular biology experiments.
Relevant literature:
Han, L., Stope, M.B., López de Jesús, M., Oude Weernink, P.A., Urban, M., Wieland, T., Rosskopf, D., Jakobs, K.H., Schmidt, M. (2007) Phospho-cofilin directly interacts with and stimulates receptor-controlled phospholipase D1. EMBO J. 26, 4189-4202
Li, X., Gao, M., Han, X., Tao, S., Zheng, D., Cheng, Y., Yu, R., Schmidt, M., Han, L. (2012) Disruption of the phospholipase D gene attenuates virulence of Aspergillus fumigatus. Infection & Immunity, 80, 429-440.
Chen, F., Zhang, C., Jia, X., Wang, J., Chen, Y., Zhao, J., Tain, S., Han, X., Han, L. (2015) Transcriptome profiles of human lung epithelial cells A549 interacting with Aspergillus fumigatus by RNA-Seq. PlosOne, D.O.I.10.1371
| Last modified: | 03 October 2017 12.00 p.m. |
