Geen leven zonder lever: hoe kunnen we leveronderzoek dichter bij de mens brengen?
Promovendus Victoria Palasantzas werkt zowel bij de afdeling kindergeneeskunde als de afdeling genetica. Daar onderzoekt ze de effecten van voedingsstoffen als antioxidanten en vetzuren op (het tegengaan van) leververvetting. Daarbij gebruikt ze het geavanceerde lever-op-chip model: een hot topic in de medische wereld.
Door Victoria Palasantzas / Foto's: Henk Veenstra
Als masterstudent droomde ik ervan mijn twee grootste wetenschappelijke interesses te combineren: de invloed van dieet op ziektebeelden en de ontwikkeling van modelsystemen waarvoor geen dieren nodig zijn. Ik kreeg de kans mijn ideeën op papier te zetten, mijn voorstel te verdedigen voor een commissie en haalde een onderzoekbeurs binnen om dit voorstel uit te voeren, met dank aan mijn begeleiders, prof. dr. Jingyuan Fu, prof. dr. Hans Jonker en prof. dr. Sebo Withoff. Doordat ik op twee verschillende afdelingen werk, zijn mijn dagen enorm afwisselend qua type werk en teams van collega’s. De ene dag kweek ik levercellen, ook wel hepatocyten genoemd, om leververvetting te bestuderen, terwijl ik de andere dag probeer zelf hepatocyten te creëren uit stamcellen.

De rol van de lever
Centraal in mijn promotieonderzoek staat de lever, de ‘multitasker’ van ons lichaam. De lever is verantwoordelijk voor de aanmaak van gal, een stof die essentieel is voor de vertering van voedsel in onze darmen. Tevens maakt de lever verschillende ‘stollingsfactoren’ aan, dit zijn eiwitten die dienen om bloedingen te stelpen. De lever speelt ook een cruciale rol in het ontgiften van onder meer geneesmiddelen en andere toxische stoffen in het lichaam. Elke persoon heeft zelfs een andere reactie hierop door zijn of haar genetische opmaak, wat leidt tot verschillende activiteit van de detoxificatie-enzymen die verantwoordelijk voor de ontgifting zijn. Daarnaast speelt de lever ook een belangrijke rol in de stofwisseling van suikers, vetten en eiwitten en daarmee de energiehuishouding van het lichaam. Door de vele functies kun je je voorstellen dat het grote impact heeft op je gezondheid, als daar iets fout gaat. Daarom is het enorm belangrijk dat we onderzoek doen naar dit fascinerende orgaan en zijn rol in gezondheid en de ontwikkeling van ziektes.

Nabootsen van leververvetting
Tijdens mijn onderzoek houd ik mij voornamelijk bezig met leververvetting, in de medische wereld ook wel bekend als MASLD (metabole stoornis-geassocieerde steatotische leverziekte) en ontstekingen als gevolg daarvan. Dit ziektebeeld gaat vaak gepaard met ongezonde leefstijlfactoren, zoals een chronisch verhoogde inname van vet en suiker en fysieke inactiviteit. Laten we naar de basis van onze stofwisseling gaan om uit te leggen wat vetophoping is. Na een maaltijd worden voedingstoffen zoals vetten opgenomen in onze darmen en daarna in de bloedstroom. Via het bloed bereiken voedingsstoffen de verschillende organen waar deze stoffen nodig zijn. Daarnaast maakt ons lichaam zelf ook vetten aan die in ons bloed terecht komen. Wanneer er een ‘overvloed’ is van deze vetten, hopen ze zich op in de lever. Klinisch gezien is er vanaf 5-10% vet van de totale leverinhoud sprake van leververvetting.

Ontstekingsreactie
Door een modelsysteem te ontwikkelen wil ik onderzoeken hoe de hepatocyten omgaan met deze overvloed aan vetten en of deze cellen nog wel hun ‘normale’ taken kunnen doen, zoals het afgeven van vetten, en hoe ze daarin verhinderd worden. Tevens zorgt leververvetting op lange termijn ook voor complicaties, waaronder ontstekingen in de lever. De hepatocyten raken gestresst en kunnen zelfs sterven, wat vervolgens leidt tot de afgifte van signalen dat er iets misgaat. Hierdoor worden immuuncellen, die ons lichaam beschermen tegen infecties en ziekten, aangetrokken naar de lever en geactiveerd. Met name macrofagen, imuuncellen die een infectie omsingelen en vernietigen, spelen hierin een rol. Om de interactie tussen hepatocyten en macrofagen beter te bestuderen probeer ik beide cellen in hetzelfde systeem te krijgen, zodat we kunnen onderzoeken wat er gebeurt tijdens deze ontstekingsreactie en welke genen of mechanismen hierbij betrokken zijn.

Het lever-op-chip model
Het liefst zou je natuurlijk de lever van een mens voor onderzoek willen gebruiken. Maar dat gaat niet zomaar, vanwege de ligging in het lichaam en de invasieve procedure. Daarom maak ik gebruik van een nieuwe state of the art technologie: het liver-on-chip model, dat qua complexiteit een stapje dichter bij de humane lever staat dan de traditionele celkweek in petrischalen. Een lever-op-chip model houdt in dat er menselijke cellen, in dit geval hepatocyten, op een chip aangebracht worden. Dit kunnen hepatocyten van gezonde donors zijn of van patiënten met een onderliggend ziektebeeld. Deze levende levercellen worden voorzien van een constante nutriëntenstroom die er, net zoals het bloed in het lichaam, voor zorgt dat er zuurstof wordt aangevoerd en afvalstoffen worden afgevoerd (zie hieronder). Hierdoor wordt een omgeving gecreeërd waarin de cellen langer in leven kunnen blijven buiten het lichaam. Er kunnen naast hepatocyten ook andere cellen, zoals immuuncellen, aan worden gebracht om de interactie tussen celtypen te bestuderen. Tussen deze celtypen zit een poreus membraan waardoor de cellen van beide kanten met elkaar kunnen communiceren door middel van signaalstoffen. Mede hierdoor kan de situatie in het menselijk lichaam goed worden nagebootst. Hierdoor kunnen we veel dichter bij de werkelijkheid komen zonder proefdieren te gebruiken.
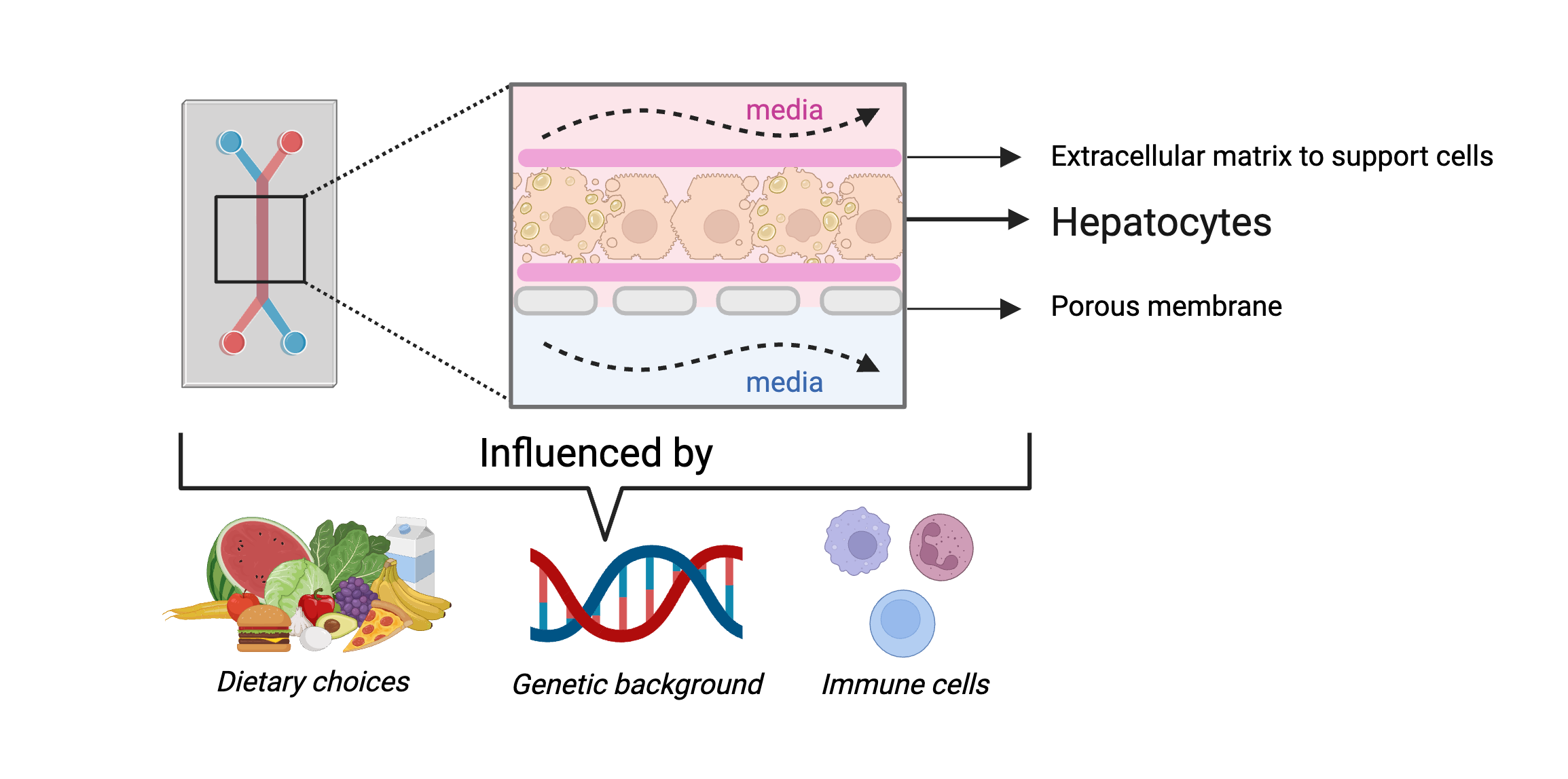
Vooruitgang
In mijn promotieonderzoek werk ik in de groep van prof. dr. Jingyuan Fu aan de ontwikkeling van het ‘lever-op-chip’ model in nauwe samenwerking met Isabel Tamargo, Gwen Weijer en dr. Joanne Hoogerland. We werken daarbij samen met de Nederlandse Organ-on-a-chip Initative (NOCI) en the Human Organ and Disease Model Technologies (hDMT). Hiervoor gebruiken wij stamcellen uit de gezonde mens, om precies te zijn humaan geïnduceerde pluripotente stamcellen (iPSCs). Deze stamcellen zijn nog niet ontwikkeld tot volwassen cellen, wat betekent dat wij ze van een ongespecialiseerde cel veranderen in een hepatocyte-achtige gespecialiseerde cel. Hierbij komt een langdurig protocol kijken van circa 40 dagen, waarin we deze stamcellen door verschillende stadia van ontwikkeling laten gaan met behulp van bepaalde factoren voordat ze hepatocyte-achtige cellen genoemd mogen worden. Een belangrijke uitdaging hierbij is ervoor te zorgen dat ze functioneel lijken op ‘volwassen’ hepatocyten, zoals de hepatocyten die je in onze levers vindt. Bij het kweken van cellen die van origine stamcel zijn kan het probleem zijn dat deze cellen meer ‘foetale’ eigenschappen hebben en niet altijd de volwaardige kenmerken vertonen van het gewilde celtype. Weet je nog die detoxificerende genen die van persoon tot persoon anders zijn, zoals eerder genoemd? In vele celmodellen van hepatocyten komen die slecht tot expressie, zoals genen van de specifieke cytochroom P450-familie (bijvoorbeeld CYP3A4). In ons liver-op-chip model proberen wij daarom de expressie en activiteit van deze genen te verbeteren.
Voeding als medicijn?
Vanuit mijn interesse naar dieet en ziekte wil ik uiteindelijk de rol van voeding op leververvetting bestuderen. Hierbij onderzoek ik specifiek de effecten op leververvetting van een aantal stoffen in onze voeding met een bekende medische werking, die ook wel nutraceutica genoemd worden. Hieronder vallen onder andere antioxidanten, die gezonde cellen en weefsels beschermen, en korte-keten vetzuren, die dienen als signaalmoleculen en energiebron voor je darmen. Veel dierstudies beschrijven positieve effecten van dit soort stoffen, al kunnen we daar in de mens nog weinig concreet bewijs voor vinden. De vervolgstappen van mijn onderzoek zullen dan ook zijn om deze nutraceutica, maar ook bekende MASLD-geneesmiddelen, die momenteel ontwikkeld worden (zoals ‘obeticholic acid’) in de lever-op-chip te gebruiken en te kijken of deze een invloed hebben op vetophoping en ontstekingen in de lever. Kortom, met mijn onderzoek hoop ik de wetenschap dichterbij de mens te brengen met behulp van het gebruik van stamcellen en het lever-op-chip model.
