ATN Blog - No mother should die while giving life!

Sisay Alemu (s.m.alemu umcg.nl) is a Ph.D. candidate at the Global Health Unit, Graduate School of Medical Sciences (RUG). He has a background in Midwifery, Mental Health, and Epidemiology. His thesis focuses on spatial inequalities in maternal and newborn health in Ethiopia. His Ph.D. is supervised by Prof. Jelle Stekelenburg (Global Health Unit, UMCG), Dr. Regien Biesma-Blanco (Global Health Unit, UMCG), Dr. Gerd Weitkamp (Faculty of Spatial Sciences, RuG), and Dr. Abera Tura (Haramaya University, Ethiopia).
Maternal and newborn babies' death is very high in sub-Saharan African countries like Ethiopia. For example, the chance of a woman dying from pregnancy-related complications in Ethiopia is 216 times higher than a similar woman in the Netherlands1. An estimated 11,000 maternal and 99,000 newborn deaths occur each year2, 3. Additionally, there is an inequitable distribution of maternal and newborn babies' health by place of residence, education, and socioeconomic status4. In fact, maternal health services utilization inequality in Ethiopia is one of the highest in the world5.
Most maternal and newborn deaths in Ethiopia can be prevented if women and babies get timely health services of good quality. However, utilization of maternal health services in Ethiopia remains a significant challenge. For example, in 2019, only 43% and 50% of pregnant women in Ethiopia received optimal pregnancy checkups and gave birth in a health facility, respectively6; and only 18% of women with pregnancy-related complications reach a facility that provides emergency maternal and newborn care7. Therefore, there is a need to increase maternal and newborn health services availability, accessibility, and utilization in Ethiopia to reduce preventable maternal and newborn deaths.
Nevertheless, scaling up health services nationwide might be expensive for low-income countries such as Ethiopia. Thus, focusing on areas where death is prevalent might be critical to effectively utilize scarce resources to save as many lives as possible. Studies indicated that interventions implemented in high risk areas (such as rural areas and low socioeconomic neighborhoods) could save up to eight times more maternal and newborn lives than when implemented in other areas8. Such an approach also helps reduce the inequality in maternal and newborn health. Hence, mapping geographic areas where maternal and newborn babies' death is predominant is crucial.
A geospatial analysis technique, among other applications, helps to illustrate how events such as death are distributed geographically. This analysis allows one to identify geographical inequalities in maternal and newborn health by locating areas where death is significantly higher than in the rest of the country. It can also help determine the possible reasons for such disparities9. As a result, findings from the geospatial analysis can improve decision-making by helping target intervention programs to areas where maternal and newborn deaths are most likely to occur.
My Ph.D. thesis focuses on using geospatial analysis to locate and prioritize areas where death is rampant so as to effectively utilize scarce resources to save as many lives as possible. The thesis answers questions such as: Where do most mothers and babies die in Ethiopia? Why do most mothers and babies die in some parts of Ethiopia more than others? With the limited resources, which geographical areas should be prioritized so that the maximum possible deaths will be prevented with the available resources?
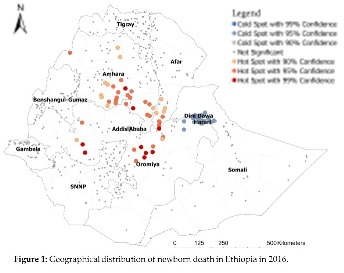
So far, we have identified geographic areas in Ethiopia where significant maternal and newborn death occur (figure 1). To answer why, I will go back to Ethiopia, specifically to the areas where most mothers and newborns die, to collect more data. Of course, this is just a small selection of my work. Do not hesitate to contact me for additional information, questions, or remarks.
This blog was made possible by the Aletta Talents Network. If you would like to contribute a blog for the ATN, please contact Tom at t.a.lowe rug.nl.
Click here to join the Aletta Talents Network!
References
- Lifetime risk of maternal death (1 in: rate varies by country) [Internet]. World Development Indicators, The World Bank Group,. 2022 [cited 29/06/2022]. Available from: https://data.worldbank.org/indicator/SH.MMR.RISK.
- World Health O, World B, United Nations Population F, United Nations Children's Fund. Trends in maternal mortality: 1990-2015: estimates from WHO, UNICEF, UNFPA, World Bank Group and the United Nations Population Division. Geneva: World Health Organization; 2015 2015.
- UNICEF W, World Bank Group, Nations U. Levels and trends in child mortality 2020: estimates developed by the UN Inter‐agency group for child mortality estimation. UN Children's Fund, World Health Organisation, World Bank and United Nations …; 2020.
- Bobo FT, Yesuf EA, Woldie M. Inequities in utilization of reproductive and maternal health services in Ethiopia. International Journal for Equity in Health. 2017;16(1):105.
- Mind the gap: equity and trends in coverage of maternal, newborn, and child health services in 54 Countdown countries. The Lancet. 2008;371(9620):1259-67.
- Central Statistical Agency - CSA/Ethiopia, ICF. Mini Demographic and Health Survey 2019. Addis Ababa, Ethiopia: CSA and ICF; 2019.
- Ethiopian Public Health Institute AMD, Disability. Ethiopian emergency obstetric and newborn care (EmONC) assessment 2016. Ethiopian Public Health Institute, Federal Ministry of Health, Columbia …; 2017.
- Ruhago GM, Ngalesoni FN, Norheim OF. Addressing inequity to achieve the maternal and child health millennium development goals: looking beyond averages. BMC Public Health. 2012;12:1119.
- Banda M, Kazembe L, Lewycka S, King C, Phiri T, Masache G, et al. Spatial modelling of perinatal mortality in Mchinji, Malawi. Spat Spatio-temporal Epidemiol. 2016;16:50-8.



