Study shows how genes affect immunity in response to pathogens
A study that is first in its kind and published in Nature Medicine today has looked at how far genetic factors control the immune cell response to pathogens in healthy individuals. A team investigated the response of immune cells from 200 healthy volunteers when stimulated with a comprehensive list of pathogens ex vivo (outside the human body), and has correlated these responses with 4 million genetic variants (SNPs). The study was performed by scientists from University Medical Centre Groningen, Radboud University Medical Centre (both in the Netherlands) and Harvard Medical School (Boston, USA). The paper appeared on 4th July 2016.
We all encounter pathogens on a daily basis, but we don’t all defend ourselves against bacteria or fungi, for example, in the same way. Some people experience mild symptoms, others may become violently ill or even die. ‘We wanted to discover how much individual genetic differences determine this variable response’, said Dr. Vinod Kumar, assistant professor of functional genomics and infectious diseases at University Medical Centre Groningen (UMCG) and one of the senior authors of the paper.
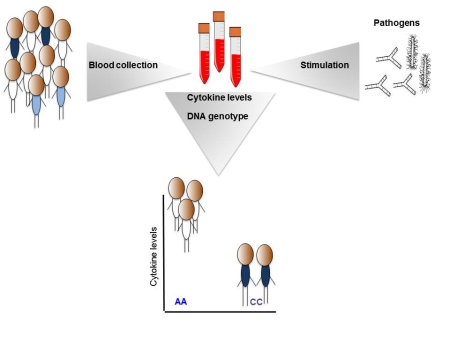
The study focused on the role of cytokines, small peptides used by immune cells as signals to guide their response to an infectious agent. Blood samples were obtained from 200 participants in the Human Functional Genomics Project, which was initiated by Professors Mihai Netea and Leo Joosten (Radboud UMC) and Prof. Cisca Wijmenga (UMCG). Immune cells were isolated from the blood and stimulated in the laboratory with ten different bacterial and fungal pathogens. The responses of eight different cytokines were measured after 24 hours and/or 7 days. Further quality filtering resulted in 62 different combinations.
‘We observed large differences in cytokine production between individuals’, explained Kumar. ‘Their responses were also specific to the different pathogens’. This suggests that cytokines contribute to the varied responses to pathogens, and that each infection triggers a specific cytokine response pathway. Previous studies on unstimulated immune cells had shown little variation between individuals.
Dr. Yang Li, another author on the study, explained: ‘The key to our results is that we performed a large-scale study, using many pathogens and measuring different cytokines’. The next step was to investigate if the responses were under genetic control. In a subset of participants, they tested 4 million single nucleotide polymorphisms (SNPs).
This pinpointed six genomic regions that influence cytokine responses, suggesting that cytokine production is at least partly genetically determined. One of the strongest examples is a SNP that affects the expression of the GOLM1 gene, which is known to express strongly in response to viral infections. In this case, there was a strong correlation with the response to the fungus Candida albicans, which is responsible for thousands of deaths each year. ‘When a particular variant of the SNP was present, the production of the cytokine interleukin-6 was reduced’, said Kumar. The result was verified in a cohort of patients with candidemia, in which the fungus is present in the blood. The candidemia correlated strongly with the same SNP and with low levels of interleukin-6 in these patients, showing that the presence of the genetic variant results in an inability to clear the pathogen.
‘This study is a real proof-of-concept’, says Li. ‘We found a lot of variation in cytokine production upon stimulation, and showed that an important part of this variation is explained by a genetic component’. This opens the way for more applied studies that move towards personalized medicine. It might well be possible to find genetic markers that will predict the risk of infection in individuals. An understanding of the genetic mechanisms underlying these different susceptibilities could lead to new therapeutic approaches.
‘And it’s not just for infections’, said Kumar: ‘Autoimmune diseases, for example inflammatory bowel disease, appear to be caused by an over-responsive immune system. So this work means we can learn more about the way infections trigger autoimmune diseases.’
Article: Inter-individual variability and genetic influences on cytokine responses to bacteria and fungi. Yang Li, Marije Oosting, Patrick Deelen, Isis Ricaño-Ponce, Sanne Smeekens, Martin Jaeger, Vasiliki Matzaraki, Morris Swertz, Ramnik Xavier, Lude Franke, Cisca Wijmenga, Leo Joosten, Vinos Kumar and Mihai Netea, Nature Medicine, 4 July 2016, doi:10.1038/nm.4139
More on the Human Functional Genomics Project: http://www.humanfunctionalgenomics.org
More about the research groups: Systems Genetics and Genetics department (UMCG); Radboud UMC/Internal Medicine, and Harvard Medical School
Contact: Vinod Kumar, email: v.kumar umcg.nl or Yang Li, email: y.li01 umcg.nl
Abstract: Little is known about the inter-individual variation of cytokine responses to different pathogens in healthy individuals. To systematically describe cytokine responses elicited by distinct pathogens and to determine the effect of genetic variation on cytokine production, we profiled cytokines produced by peripheral blood mononuclear cells from 197 individuals of European origin from the 200 Functional Genomics (200FG) cohort in the Human Functional Genomics Project (http://www.humanfunctionalgenomics.org), obtained over three different years. We compared bacteria- and fungi-induced cytokine profiles and found that most cytokine responses were organized around a physiological response to specific pathogens, rather than around a particular immune pathway or cytokine. We then correlated genome-wide single-nucleotide polymorphism (SNP) genotypes with cytokine abundance and identified six cytokine quantitative trait loci (QTLs). Among them, a cytokine QTL at the NAA35-GOLM1locus markedly modulated interleukin (IL)-6 production in response to multiple pathogens and was associated with susceptibility to candidemia. Furthermore, the cytokine QTLs that we identified were enriched among SNPs previously associated with infectious diseases and heart diseases. These data reveal and begin to explain the variability in cytokine production by human immune cells in response to pathogens.
Kennis in Zicht artikel (in Dutch)
Persbericht/press release (in Dutch)
| Last modified: | 24 April 2024 2.04 p.m. |
More news
-
16 April 2024
UG signs Barcelona Declaration on Open Research Information
In a significant stride toward advancing responsible research assessment and open science, the University of Groningen has officially signed the Barcelona Declaration on Open Research Information.
-
02 April 2024
Flying on wood dust
Every two weeks, UG Makers puts the spotlight on a researcher who has created something tangible, ranging from homemade measuring equipment for academic research to small or larger products that can change our daily lives. That is how UG...
-
18 March 2024
VentureLab North helps researchers to develop succesful startups
It has happened to many researchers. While working, you suddenly ask yourself: would this not be incredibly useful for people outside of my own research discipline? There are many ways to share the results of your research. For example, think of a...
